October 11, 2017
In harm’s way: Workplace violence in health care
People go to the hospital to be cared for and get better. But for health care professionals, going to work can put them in harm’s way.
Nursing homes and hospitals are among the most high-risk occupations for injuries generally , and their rate of injuries from workplace violence are much greater than the average — 5 to 12 times higher, according to a recent Washington Post article .
According to OSHA , "health care accounts for nearly as many serious violent injuries as all other industries combined."
Defining workplace violence
Workplace violence encompasses more than physical assaults. The National Institute for Occupational Safety and Health’s definition includes threats of assault as well as verbal abuse, hostility and harassment.
This violence can be committed by co-workers, patients or family members of patients. Health care workers interact with a large number of people throughout their day, often in stressful situations.
Quantifying violent incidents in the health care sector
The most recent statistics from OSHA and the Bureau of Labor Statistics paint a picture of shocking risks to workers:
- In 2015, more than 11,000 violent incidents against employees in the health care and social assistance sector occurred
- Assaults made up 10 percent of all lost-time work injuries in health care
- Of the 24 work-related fatalities in hospitals, five were a result of “violence and other injuries by persons or animals”
- The same category of “violence and other injuries by persons or animals” accounted for 11 percent of lost-time injuries in private hospitals and a staggering 45 percent of injuries in state-run hospitals (possibly because these facilities are predominantly psychiatric and substance abuse hospitals)
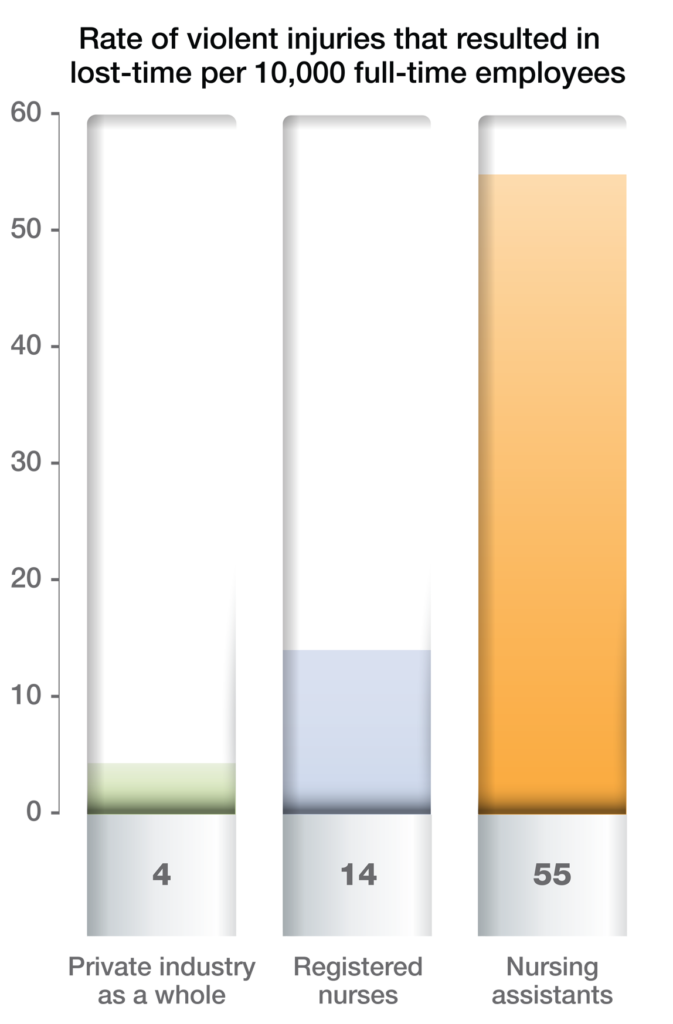
Within health care, some positions are more exposed to the risk of violence. Employees who work with patients with dementia or psychiatric issues, for example, may be at greater risk. Registered nurses and nursing assistants have higher lost-time injury rates due to violence than private industry on average.
Under-reporting workplace violence
According to OSHA’s "Workplace violence in health care: Understanding the challenge" report , violent incidents in health care often go unreported, with verbal abuse and bullying less likely to be reported than physical altercations.
A 2004 study of Minnesota nurses in the Journal of Occupational and Environmental Medicine “found that only 69 percent of physical assaults and 71 percent of non-physical assaults were reported to a manager.” The same study concluded that workplace violence — or the threat of violence — can hurt workplace morale and productivity and lead to higher burnout and turnover.
Preventing violent injuries in health care
With such a high rate of injuries in health care, OSHA updated its "Guidelines for Preventing Workplace Violence for Healthcare and Social Service workers" in 2015. The voluntary recommendations are designed for health care workers at all levels, from support staff to physicians, and in settings across the continuum of care, from home health care to hospitals.
The guidelines recommend incorporating a workplace violence prevention program into an organization’s broader safety and health program. An effective workplace violence prevention program addresses five components:
- Management commitment and employee participation
- Worksite analysis
- Hazard prevention and control
- Safety and health training
- Recordkeeping and program evaluation
OSHA’s resources include a workplace violence program assessment checklist, which covers topics such as staffing, training, facility design, security measures and workplace procedures, as well as considerations for workers who do field work. Training may include de-escalation and self-defense techniques.
With health care workers facing a real threat of workplace violence, organizations should take steps to track incidents accurately, train employees on de-escalation techniques and implement a workplace violence prevention program.
Additional resources
- SFM fact sheet: Occupational injuries in health care
- SFM De-escalation Team Training - health care
- Combative patient behaviors Supervisor Initiated Training
- OSHA: Workplace violence in healthcare: Understanding the challenge
- OSHA: Preventing workplace violence in healthcare
- American Nurses Association bullying and workplace prevention page